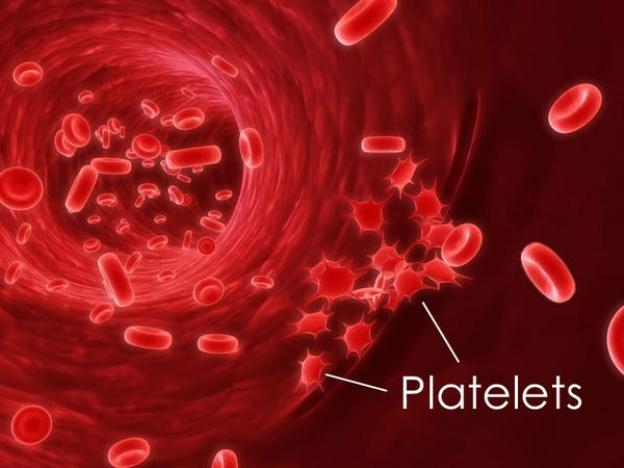
Essential Thrombocythemia is a chronic myeloproliferative neoplasm (MPN), which is characterized by an increased number of platelets in the blood. It is most common in women over the age of 50. ET is generally associated with a proliferation of platelet precursors in the bone marrow. Complications such as frequent blood clotting and/or bleeding are common.
ET typically occurs due to clonal abnormality of a multipotent hematopoietic stem cell. The location where it found mostly is bimodal peaks of between ages 50 and 70 yr and a separate peak among young females. In simple words, platelet production is increased in patients. Platelet survival is usually normal, it may decrease in some cases due to splenic sequestration or, in patients with erythromelalgia, digital ischemia.Increased platelets may lead to serious bleeding.
According to some recent studies, an elevated leukocyte count is a major independent risk factor for thromboses. Bleeding is more likely with extreme thrombocytosis due to an acquired deficiency of von Willebrand factor. If someone is suffereing from such condition, bone marrow examination is strongly recommended, especially in patients with anemia, macrocytosis, leukopenia, or evidence of extramedullary hematopoiesis. The bone marrow shows megakaryocytic hyperplasia, with an abundance of platelets being released. In order to distinguish it from other myeloproliferative disorders that cause thrombocytosis, the diagnosis of ET requires a normal Hct, MCV, and iron studies.
Essential Thrombocythemia Prognosis and Treatment
If you want to knowmore about this medical condition, then keep reading.
Causes
Despite the fact that medical science is very advance now a days, still no one knows the exact causes of essential thrombocythemia (ET) or other myeloproliferative neoplasms (MPNs). Just like many other MPNs, ET is not a genetically inherited disorder, but a familial predisposition to the disease in some patients is still important. As per researchers, mutations could be a factor that alter the activity of proteins that control signaling pathways in many patients with ET. Main risk factors include:
- Gender, as discussed above, women are mostly effected,
- Age, people with an age of 60 or above are most likely to develop ET.
- Environment, as exposure to chemicals may increase an individual's risk for ET
- Mutation, unfortunately half of all ET patients have a mutation of the JAK2 gene in their blood-forming cells.
- This mutation leads to hyperactive JAK (Janus kinase) signaling, resulting in producing wrong number of blood cells.
Diagnosis
ET can be easily deducted after a routine blood test which shows that a patient has a high platelet count. Patient can experience one or more symptoms of ET and consult physician, who can determine whether a patient has ET, after performing diagnostic tests and a review of patient history and symptoms. Common tests for diagnosing ET include:
Blood Tests
Blood tests are something that the physician recommend firstly in such case. Most common tests are for iron deficiency and indicators of inflammation as well as other mimicking blood diseases.
Bone Marrow Biopsy
A bone marrow biopsy gives an insight for classical signs of ET, such as an increase in platelet precursors.
Gene Mutation Analysis
As discussed above, sometimes a gene mutation can be responsible for such a medical condition. So gene mutation test like JAK2, CALR, MPL are also common as diagnosis tool.
Symptoms
Common symptoms include:
- fatigue, or may be related to small or large vessel disturbance or bleeding.
- Headache
- Vision disturbances
- Silent migraines
- Coldness or blueness of fingers
- Burning, redness, and pain in the hands and feet
- Easy bruising, nosebleeds or heavy periods
- Blood in the urine
- Blood clotting in unusual locations, such as the abdominal veins
- Due to clotting, stroke or heart attack can also occur
Prognosis
With proper monitoring and good treatment, thrombocythemia patients usually survive. Patients have to consult regularly with a hematologist and to report any symptoms such as visual disturbances, unexplained pain, numbness, tingling or bruising. Only a small minority of people with ET may later develop acute leukemia or postpolycythemic myelofibrosis (15%), both of which can be life threatening.
Treatments
Although there is no single treatment option that can be considered appropriate or effective for all ET sufferers, as some patients are asymptomatic and require no treatment, others may require various treatments and therapies, based on the symptoms and the results of routine monitoring by a physician. Following are some commonly used treatment options for ET patients.
- In order to reduce the risk of blood clotting, low-dose aspirin is usually given to patients. It may also help relieve the burning sensation in hands or feet.
- Hydroxyurea is most common treatment that ET patients get, who are at high risk for clotting.
- Anagrelide is an excellent option for lowering platelet counts.